The financial year of 2017/18 saw the highest number of organs ever donated in the UK. However, as organ donation figures continue to rise so too does the demand for transplants.
By 2020 a new opt-out system for organ donation could be put in place across England if parliament approves “Max’s Law”.

Access deeper industry intelligence
Experience unmatched clarity with a single platform that combines unique data, AI, and human expertise.
However, with the Medical University of Vienna 3D printing a human placenta earlier this year and biotech company BIOLIFE4D aiming to print a human heart by 2019, could 3D printed organs soon be the much-needed solution to the organ donation crisis?
Positive progress
The process of 3D printing organs involves 3D bio-printers and bio-ink. The medically designed printers contain computer-guided pipettes which can create human tissue by printing layers of bio-ink, a substance usually made from stem cells, on top of one another. Eventually, a range of tissues can be printed together to form an organ.
This technology is advancing so rapidly that 3D printed organs for use in human transplantations could be a reality sooner than we think.
BIOLIFE4D CEO Steven Morris told Verdict:
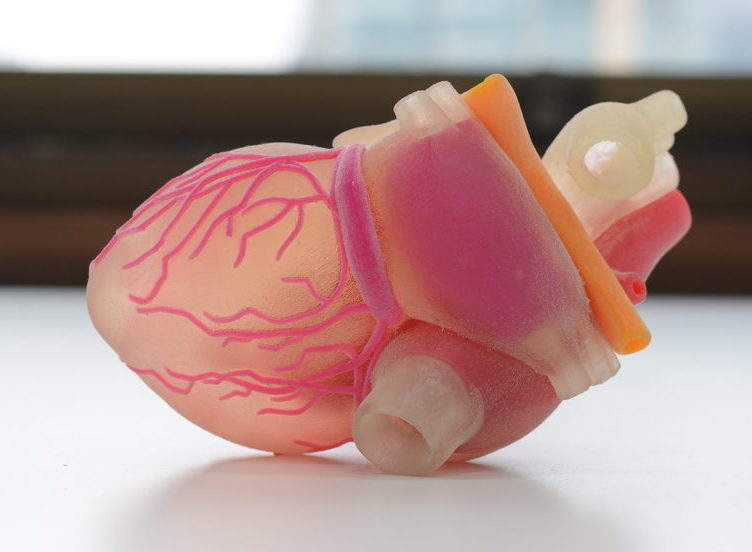
“We are actually planning to be able to 3D bio-print an organ in 2019. It will be a human heart, made out of human heart cells, but it will only be the size of a mouse heart and not viable for transplantation.
“It will, however, represent a huge step forward for BIOLIFE4D and our efforts to 3D bio-print a full sized human heart viable for transplantation using a patient’s own cells to prevent the current challenges of rejection and the need for immunosuppressant therapy as a result of a donor organ.
“Besides providing validation of our process, we believe that our ‘mini-heart’ could be a tremendously valuable tool for pharma with human predictive cardiac toxicity and efficacy models.”
Scientists at the Medical University of Vienna went a step further than BIOLIFE4D when they released a research paper in August detailing how they had 3D printed a simplified, organic model of the human placenta with the aim of studying its development.
These scientists are not alone in having created what is commonly referred to as an organ-on-a-chip device for use in pharmaceutical testing. Researchers from Wyss Institute for Biologically Inspired Engineering at Harvard University, Instituto Superior Técnico in Portugal, Boston Children’s Hospital, and Harvard Medical School collaborated to create an organ-on-a-chip model of the human gut which they say can better predict the effect of radiation exposure on humans than animal testing.
Perhaps one of the biggest drawbacks of the current 3D bio-printing technologies is that the tissues being printed can only form organoids which are smaller and simplified versions of organs. The process will therefore need to be scaled up and developed at a much more intricate level before it can reach its true potential.
The future
So, we know that 3D printed organoids made from human tissue are already a reality and are currently being used in medical testing. However, when this technology will be ready to provide an alternative to human organ donation is harder to pinpoint.
Carmat, the company working to create the world’s most advanced total artificial heart to treat biventricular heart failure, has used 3D printed tissues to partially reconstruct the hearts of 11 patients so far. These hearts need to be powered outside of the body.
The results are looking positive so far though as patients with these partial transplants have all survived over the 18th month period.
The company is planning to conduct more trials so the technology can be developed further.
BIOLIFE4D’s Morris seems positive that his company will be printing full scale models of human hearts sooner rather than later. He said:
“We are still at least a few years away from being able to scale the bioengineered heart to the size of a human heart, and there are many challenges we will face along the way.
“We are totally dedicated, however, to bringing this incredible technology to the market in the absolute shortest time possible as we know the profound impact it could have.
“With nearly 1 in every 3 people, in every developed nation around the world, dying as a result of cardiovascular disease and only about 5,000-6,000 donor heart transplants occurring globally each year, we know how many lives could be saved each year once this technology can be deployed.”







