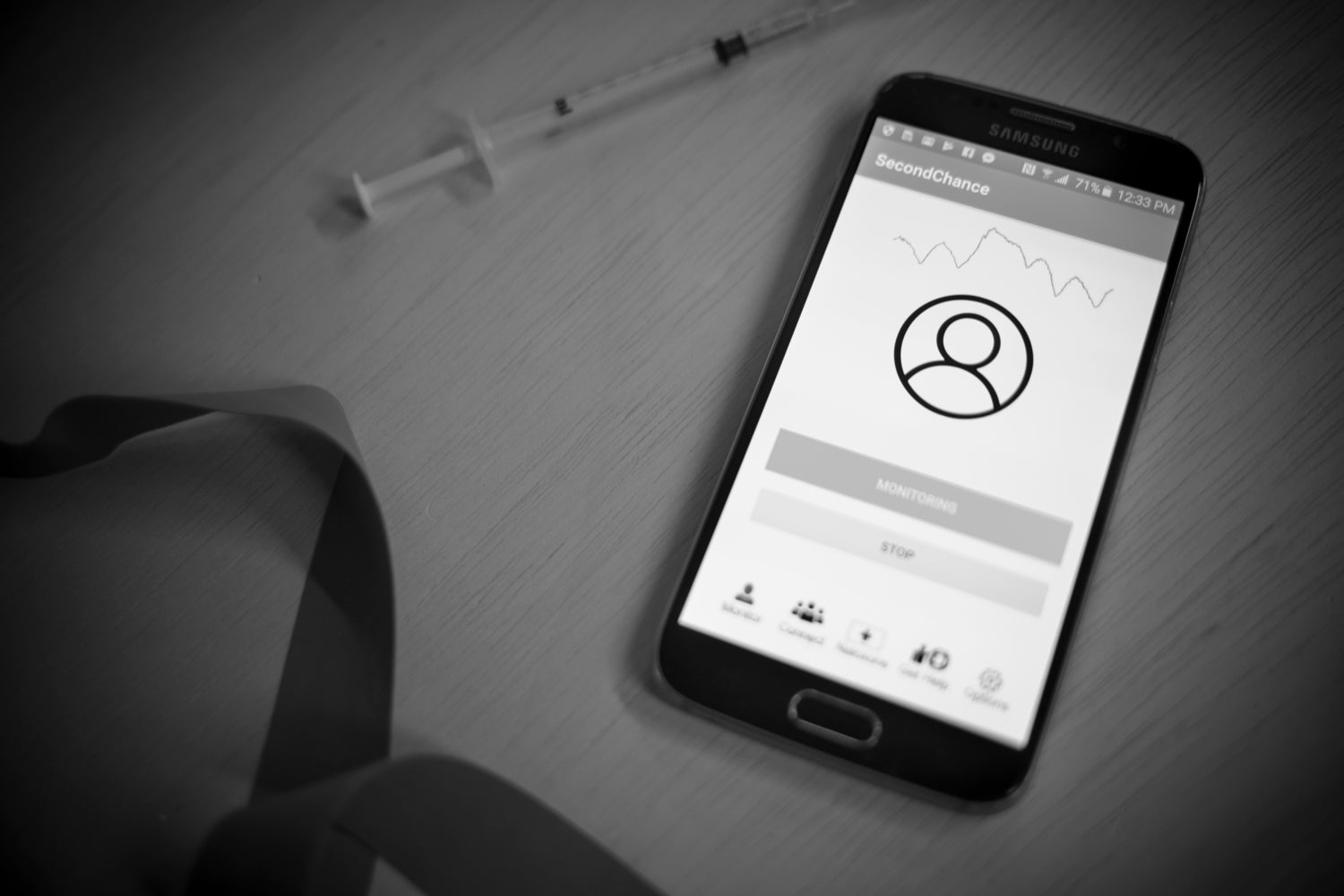
A smartphone app called Second Chance has been developed to detect overdose-related symptoms in opioid users by using sonar to monitor breathing rates.
The app sends inaudible sound waves from the phone to people’s chests, monitoring the way the sound waves return to the phone and checking for specific breathing patterns.

Access deeper industry intelligence
Experience unmatched clarity with a single platform that combines unique data, AI, and human expertise.
Second Chance also monitors how a person moves to detect possible overdosing, such as if the user’s head “slumps or nods off”.
“We’re experiencing an unprecedented epidemic of deaths from opioid use, and it’s unfortunate because these overdoses are completely reversible phenomena if they’re detected in time,” said Dr Jacob Sunshine, assistant professor of anesthesiology and pain medicine at the University of Washington’s School of Medicine.
“The goal of this project is to try to connect people who are often experiencing overdoses alone to known therapies that can save their lives. We hope that by keeping people safer, they can eventually access long-term treatment.”
The dangers of opioid use
More than 115 people die every day from overdosing on opioids in the US, according to the National Institute on Drug Abuse.
Opioids include certain prescription pain relievers, heroin and synthetic opioids such as fentanyl.
A person experiencing an overdose will find their breathing becomes slower or stops altogether.
This is reversible if the drug naloxone is administered in time, however, the person using the opioid usually has no way of asking for help if they do overdose.
Second Chance lets people use the app during opioid use and if they overdose the phone will connect them with a friend or emergency service to provide the naloxone.
“When the app detects decreased or absent breathing, we’d like it to send an alarm asking the person to interact with it,” said Shyam Gollakota, an associate professor in the University of Washington’s Paul G. Allen School of Computer Science and Engineering.
“Then if the person fails to interact with it, that’s when we say: ‘Okay this is the stage where we need to alert someone,’ and the phone can contact someone with naloxone.”
Testing Second Chance at a legal drug consumption site
The researchers at the University of Washington partnered with the Insite supervised injection facility in Vancouver, the first legal supervised consumption site in North America, to use real-world data to design and test the algorithm in the app.
“We asked participants to prepare their drugs like they normally would, but then we monitored them for a minute pre-injection so the algorithm could get a baseline value for their breathing rate,” said Rajalakshmi Nandakumar, a doctoral student in the Allen School.
“After we got a baseline, we continued monitoring during the injection and then for five minutes afterwards, because that’s the window when overdose symptoms occur.”
Half of the 94 participants testing the algorithm had a breathing rate lower than seven breaths per minute and 49 stopped breathing altogether for a significant period of time.
Two users experienced an overdose and needed oxygen, ventilation and naloxone treatment.
The researchers also worked with anaesthesiology teams to simulate overdoses in an operating room, so that they could program the app to detect actual cases of overdose and not just symptoms.
“When patients undergo anaesthesia, they experience much of the same physiology that people experience when they’re having an overdose,” Sunshine said.
“Nothing happens when people experience this event in the operating room because they’re receiving oxygen and they are under the care of an anesthesiology team. But this is a unique environment to capture difficult-to-reproduce data to help further refine the algorithms for what it looks like when someone has an acute overdose.”
The Second Chance team are applying for the US Food and Drug Administration’s (FDA) approval and plan to commercialise the tech.
So far the app has only been tested on illegal injectable opioid use, although it could be used for all forms of opioid use.







