The start of November marks the beginning of Movember, a month set aside by The Movember Foundation to raise awareness of some of the biggest health issues faced by men: prostate cancer, testicular cancer, and mental health and suicide.
The Movember Foundation describes itself as “the leading charity changing the face of men’s health”. It hopes to reduce the number of men dying prematurely in the UK by 25% by 2030.

Access deeper industry intelligence
Experience unmatched clarity with a single platform that combines unique data, AI, and human expertise.
Early this year, figures released from the UK’s Office for National Statistics reported that prostate cancer had killed more people than breast cancer in 2015. Lung, breast, prostate and bowel cancer are the most common types of cancer and account for more than half of cases in the UK.
Movember prostate cancer
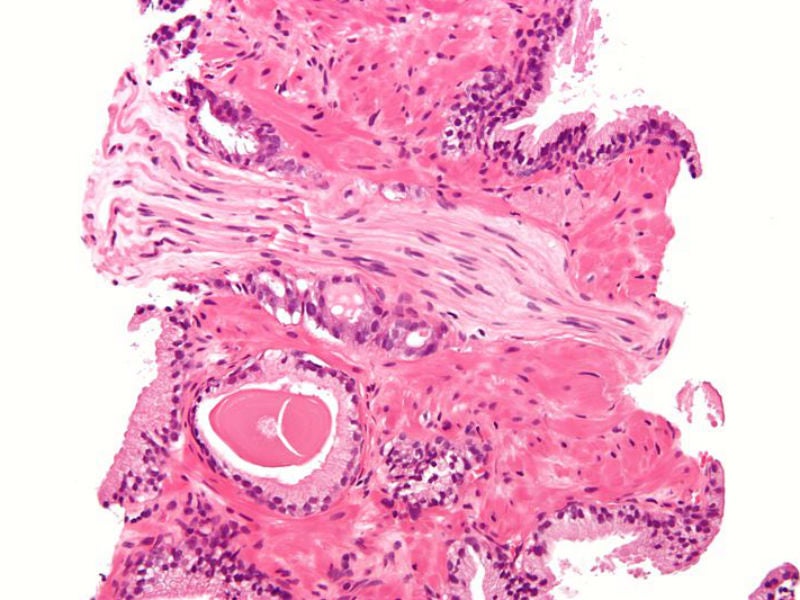
Prostate cancer is the most common cause of cancer in men. Across the UK, over 47,000 men are diagnosed with prostate cancer every year and one patient with the disease dies every 45 minutes.
The prostate is a small gland found only in the pelvis of men and has the purpose of creating a thick white fluid to create semen when combined with sperm. The cancer can develop when cells in the prostate start to grow in an uncontrolled way and sometimes spreads to other parts of the body if left untreated.
Some of the funds raised during Movember will go towards research with the aim of improving early cancer detection, diagnosis and effective treatments, and ultimately reducing the number of preventable deaths.
This year has seen a number of developments regarding medical technology solutions to improve prostate cancer diagnosis and treatment. Here are five new devices aiding prostate cancer patients and the Movember prostate cancer cause.
Blood analysis: earlier detection and prognosis

Earlier this year, a study led by the Institute of Cancer Research (ICR) found that a test used to analyse blood samples for traces of tumour cells could help to identify therapy responses in advanced prostate cancer patients.
The research involved 500 prostate cancer patients and showed that tumour cells present in samples obtained during the initial 12 weeks after the start of treatment are indicative of poorer outcomes in the future. Patients with zero circulating tumour cells in their blood samples lived for an average of more than two years following therapy.
This summer, cancer diagnostics developer VolitionRx reported positive preliminary results from a proof-of-concept clinical study of its Nu.Q assays to detect high-grade prostate cancer. The assays involve a series of blood tests to identify ‘very early’ nucleosomic markers of cancer, visible before the disease spreads.
Genomic Health has also launched a new prostate cancer-focused liquid biopsy test this year. The test is called the Oncotype DX AR-V7 Nucleus Detect, which can predict treatment response for patients suffering from metastatic castration-resistant prostate cancer (mCRPC) in the US. The test was developed by Epic Sciences using its No Cell Left Behind platform and can identify a splice variant of the androgen receptor protein (AR-V7) in the nucleus of circulating tumour cells.
Imaging for prostate cancer diagnosis and management

Researchers at the University of Dundee in the UK have identified a new imaging technique which they claim enables better diagnosis and management of prostate cancer. The imaging technique is known as shear wave elastography (SWE) ultrasound and is a non-invasive and less expensive alternative to current imaging methods. It is also said to be more accurate and reliable at detecting cancer.
Findings from an international clinical study have also revealed that undergoing an MRI scan can eliminate the need for invasive biopsies in more than a quarter of men suspected of having prostate cancer. Currently, a transrectal ultrasound-guided (TRUS) biopsy is commonly used to extract and analyse small tissue samples to find out if a patient has prostate cancer. However, this study found that MRI scanning can identify people who do not require the painful biopsy test.
Credit: University of Dundee.







