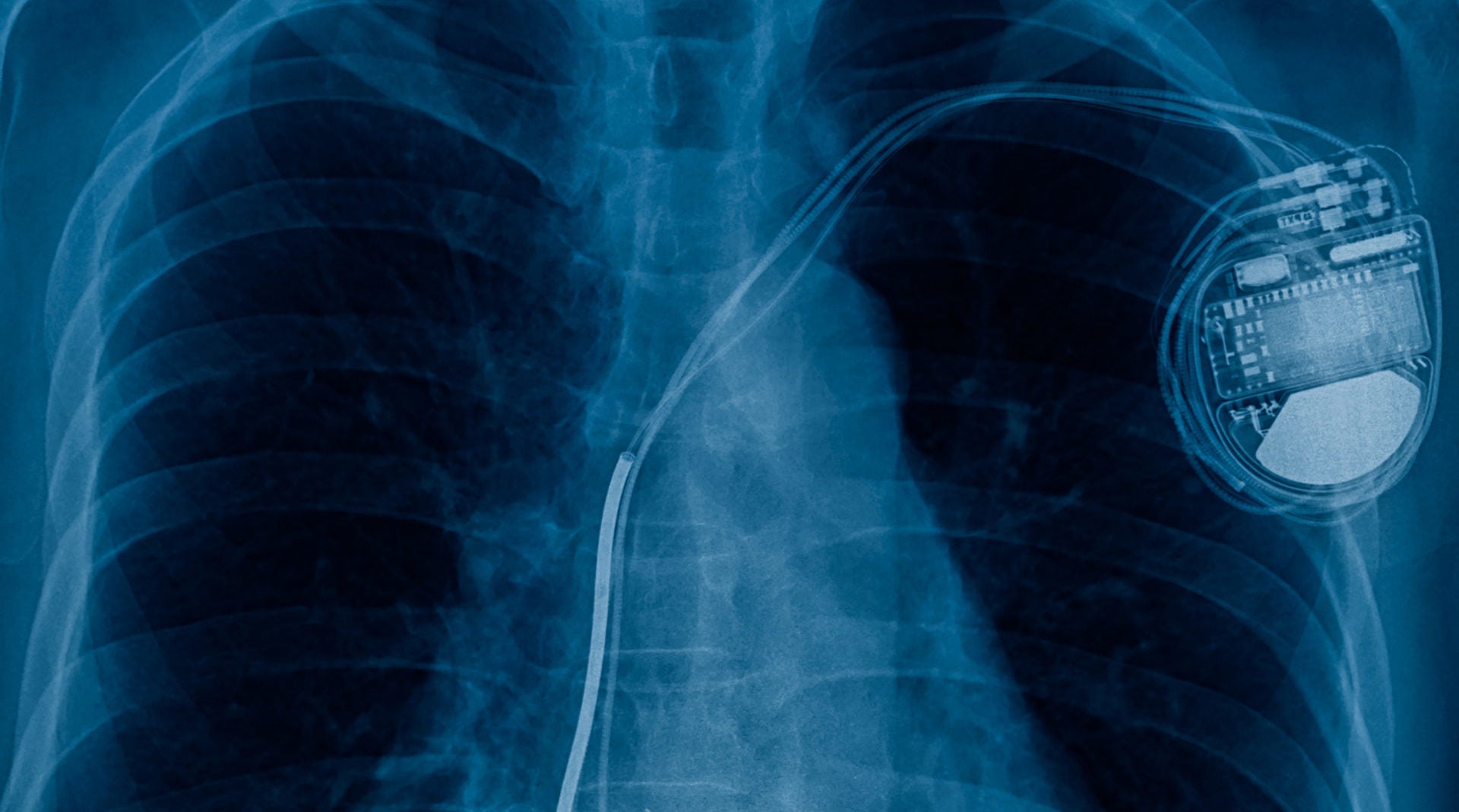
Researchers have created artificial intelligence (AI) software that identifies the make and model of cardiac rhythm devices – such as pacemakers – in seconds, massively speeding up treatment times in potentially life-threatening conditions.
Although rare, a cardiac device can malfunction, leading to heart palpitations, loss of consciousness or electric shocks. In the absence of patient records or the patient knowing the type of device, doctors currently use a flowchart algorithm to identify pacemakers via a process of elimination.

Access deeper industry intelligence
Experience unmatched clarity with a single platform that combines unique data, AI, and human expertise.
For the million-plus people around the world who have a cardiac rhythm device implanted each year, this method can be time-consuming and inaccurate.
To combat this, a research team at Imperial College London, UK, developed AI software that recognises the make and model of a cardiac device from an X-ray image alone.
After uploading the image to a computer, the AI program detects the type of device within seconds, which means patients can be diagnosed and treated at a much faster rate.
“Pacemakers and defibrillators have improved the lives of millions of patients from around the world,” said Dr James Howard, clinical research fellow at Imperial College London and lead author of the study.
“However, in some rare cases these devices can fail and patients can deteriorate as a result. In these situations, clinicians must quickly identify the type of device a patient has so they can provide treatment such as changing the device’s settings or replacing the leads.”
“Unfortunately, current methods are slow and out-dated and there is a real need to find new and improved ways of identifying devices during emergency settings.”
Training the AI pacemaker software
Researchers used a neural network, a type of machine learning that is modelled on the human brain and nervous system, to create the cardiac device recognition software.
Because it can identify over 1,600 different types of cardiac devices, it would have had to be trained on many times this amount of images, with slight variations of each device.
When the team tested the software on over 1,500 radiographic images from patients at Hammersmith Hospital between 1998 and 2018, they found the software outperformed traditional identification methods.
Where the current flowchart method was accurate for 72% of the time, the Imperial College London software was 99% accurate.
“Our new software could be a solution as it can identify devices accurately and instantly,” said Dr Howard. “This could help clinicians make the best decisions for treating patients.”
Before the software can be used in hospitals the researchers will need to carry out further trials to validate the findings among a larger group of patients. They also plan to explore ways to make a more portable device that can be easily transported around hospital wards.
The study was conducted at Hammersmith Hospital, which is part of Imperial College Healthcare NHS Trust. The findings were published in the scientific journal JACC: Clinical Electrophysiology.
Read more: Google Home medical app aids physicians during surgery







